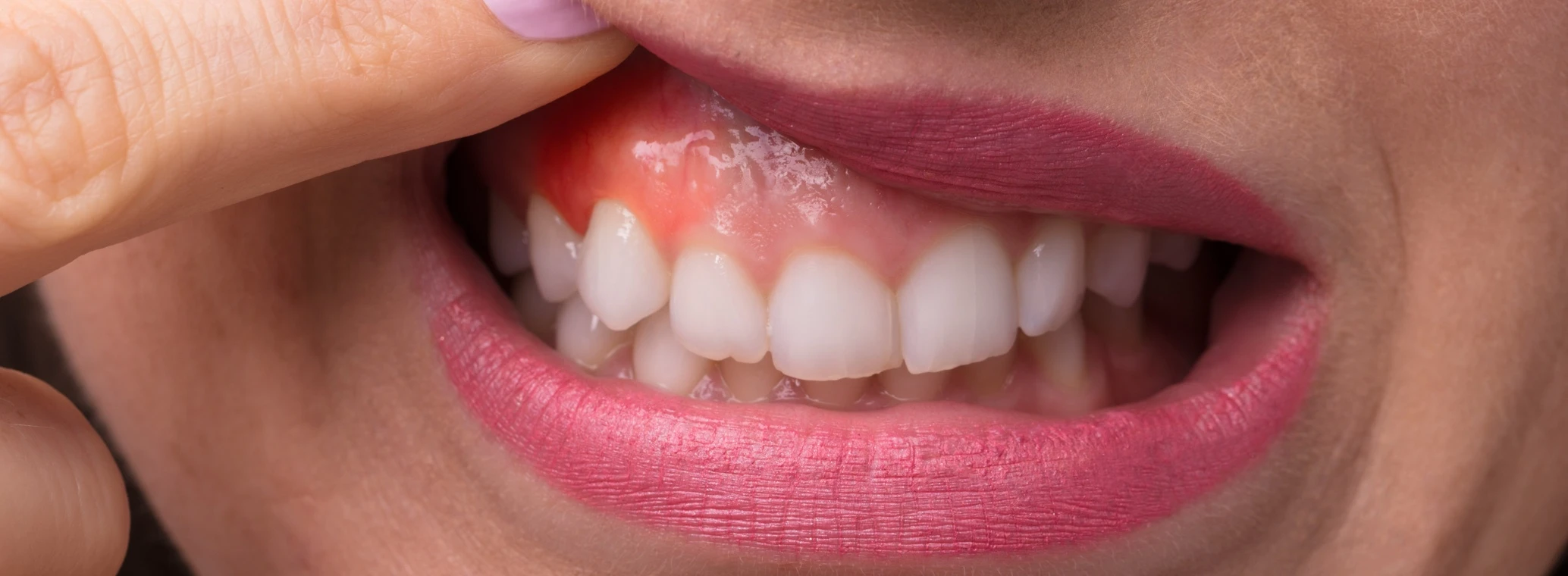
Gum-Health
Gum Pain: Causes, Relief, and Treatment
Beyond mere discomfort, gum pain can signal a more significant underlying dental problem. How can you determine if the sensations you're experiencing require an urgent dental consultation?
This article will explore the various potential triggers of gum discomfort, the accompanying signs, and effective approaches to alleviate your pain.
KEY TAKEAWAYS
TABLE OF CONTENTS

TABLE OF CONTENTS
What Leads to Gum Discomfort?
- Poor Oral Hygiene: Inadequate oral hygiene stands as the primary instigator of gum pain. Insufficient brushing and flossing allow plaque to accumulate along the gumline, gradually eroding tooth enamel and ultimately paving the way for infection.
- Gum Disease: Periodontal disease frequently develops in sequential phases, beginning with gingivitis and escalating to the more severe condition of periodontitis. Gingivitis, the initial phase of gum disease, is recognizable by red, swollen, and bleeding gums. Fortunately, with diligent oral hygiene, this stage is reversible. Periodontitis, the more advanced and serious phase, involves gum recession, loss of supporting bone structure, and loosened teeth. Unlike gingivitis, periodontitis is an irreversible condition.
- Vitamin Deficiency: Insufficient intake of vitamin B and vitamin C within your diet may result in inflamed and tender gums, among other issues like fatigue, headaches, mood disturbances, and memory difficulties. Such nutritional shortfalls are more common when a person's diet lacks adequate fruits, vegetables, and lean protein, deviating from healthy eating recommendations.
- Hormonal Changes: Fluctuations in hormone levels can also trigger gum discomfort. Although both sexes can be affected, women often exhibit greater susceptibility due to hormonal changes occurring during puberty, menstrual cycles, gestation, and menopause. Elevated blood flow and hormonal adjustments during pregnancy can lead to pregnancy gingivitis in some expectant mothers.
- Abscessed Tooth: An infection can occasionally develop beneath the gumline, adjacent to a tooth's root. This condition is termed a dental abscess. Abscesses commonly present as swollen, tender gums due to the inflammatory response and pressure exerted on surrounding tissues by the infection. Neglected abscesses can result in severe complications, including widespread systemic infections. Therefore, if you observe a swollen area on your gums, seek immediate dental attention. Your dentist can accurately diagnose the issue and propose an appropriate treatment plan.
Indicators Often Associated with Gum Discomfort

Prior to delving into additional signs that may accompany gum discomfort, remember that these symptoms can point to deeper health issues. Should you experience intense gum pain, pain persisting for over a week, a fever, or any other worrying symptoms, consult a dentist without delay.
- Tenderness and Swelling: As previously mentioned, sensitivity and inflammation frequently co-occur with gum discomfort. These symptoms usually arise from a subgingival infection, which exerts pressure on the adjacent tissues. This same tenderness and swelling can also be a localized reaction to food debris, such as popcorn kernels, becoming trapped along the gumline.
- Bright or Dark Red Gums: Upon the onset of infection, your body's immune response directs increased blood flow to the affected region in an effort to promote healing. This process can cause your gums to take on a vivid or deep red hue. If you observe such discoloration, particularly when combined with other symptoms detailed here, schedule an immediate dental visit.
- Bleeding: Occasional gum bleeding might occur, often following flossing or consuming abrasive foods that irritate the gum tissue. Nonetheless, if your gums bleed without an apparent cause, it is advisable to arrange a dental appointment to ascertain the underlying issue.
- Pain When Chewing: The act of chewing places mechanical stress on your teeth and gums. Should an issue exist beneath the gumline, this pressure will intensify any existing gum discomfort. This serves as a strong incentive to consult your dentist, ensuring that the root cause of the pain does not propagate to adjacent teeth or jawbone structures.
- Loose Teeth: Significant issues developing below the gumline have the potential to compromise the critical supporting components of your teeth, including nerves, roots, and bone. This damage can lead to mobile or "wiggly" teeth. Consistent with other indicators, if you perceive that your teeth are loose, arrange an immediate dental consultation.
Managing Gum Discomfort: Treatment Options
See a Dentist: When confronted with dental pain, consulting a dentist is your optimal course of action. They possess the expertise to determine the most effective solution for your condition. Nevertheless, certain measures can be taken at home. Let's explore them.
Improve Oral Hygiene: Implement strategies to enhance your oral hygiene. Generally, this includes:
- Brushing your teeth at least twice daily with a dentist-recommended stannous fluoride toothpaste and an electric toothbrush.
- Flossing once daily.
- Rinsing with a gum detoxifying mouthwash.
- Saltwater rinse: Dissolve one teaspoon of salt in one cup of warm water. Take a mouthful of the mixture and swish it thoroughly around your teeth and gums. Expel the water. Repeat this process until the water is used up.
- Cold compression: Saturate a washcloth in cold water and apply it to the tender region. Alternatively, an ice cube wrapped in a cloth can be used.
- Over-the-counter pain medication: Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or aspirin can aid in reducing inflammation and mitigating gum pain. It's crucial to remember that these medications provide symptomatic relief but do not address the core issue.
Take Care of Your Gums with Crest and Oral-B

Healthy gums are indispensable for overall tooth and mouth health. In the presence of gum disease, the initial and most crucial step is to consult a dental professional. They can conduct a thorough examination, ascertain the severity of the disease, and recommend appropriate treatments. However, there are also proactive measures you can take.
- Toothpastes containing stannous fluoride, like the Crest Gum Detoxify Toothpaste line, are formulated to target and neutralize the harmful plaque bacteria that accumulate around the gumline and cause gingivitis.
- Some mouth rinses, such as Crest Pro-Health Multi-Protection Mouthwash, are clinically proven to offer 24-hour protection against plaque and gingivitis when used twice daily.
- When you brush with Oral-B iO electric toothbrushes, their gentle micro-vibrations and smart pressure sensor help you achieve an effective clean while simultaneously protecting your gums. A study demonstrated that for individuals prone to gingival recession, an electric toothbrush proved to be a safe choice over a 36-month period.
- Selecting the right brush head also significantly contributes to effective cleaning without causing gum irritation. Therefore, complement your toothbrush with an advanced brush head, such as the Oral-B Gentle Care brush head, which is specifically designed for a gentle yet highly effective clean along the gumline.
- Seek a Dental floss, that resists shredding and glides effortlessly into constricted areas, such as Oral-B Glide Pro-Health Comfort Plus Floss.
TABLE OF CONTENTS

TABLE OF CONTENTS
WE RECOMMEND
FAQs

How can I relieve gum pain?
The most effective method for alleviating gum discomfort is to consult your dentist, who can pinpoint the pain's underlying cause. While awaiting your appointment, you may attempt one or all of the following tactics:
• Swish with warm saltwater (1 teaspoon of salt in 1 cup of water) every two hours.
• Apply a cold compress to the affected region.
• Utilize an over-the-counter pain reliever.
• Swish with warm saltwater (1 teaspoon of salt in 1 cup of water) every two hours.
• Apply a cold compress to the affected region.
• Utilize an over-the-counter pain reliever.

Why do I have gum pain after flossing?
Improper flossing techniques can occasionally lead to gum soreness and irritation. To prevent this, always floss with a gentle touch. Rather than forcefully moving the floss into your gum line, carefully guide it up and down along each tooth surface. You might also consider opting for waxed dental tape over unwaxed floss, as it tends to fray less and cause less gum irritation.

Can a gum infection heal itself?
Whether a gum infection resolves spontaneously depends on its root cause. Minor gum discomfort or early-stage gum inflammation (gingivitis) may sometimes heal naturally. However, more severe gum infections, like periodontitis or an abscess, typically necessitate professional medical intervention. To aid in the recovery of minor gum discomfort and irritation, implement these measures:
• Brush and floss daily.
• Use an antibacterial mouthwash.
• Cease smoking.
• Maintain a balanced diet rich in fruits, vegetables, and lean protein.
• Minimize stress.
If gum pain endures or if signs of an infection become apparent, seek dental consultation without delay.
• Brush and floss daily.
• Use an antibacterial mouthwash.
• Cease smoking.
• Maintain a balanced diet rich in fruits, vegetables, and lean protein.
• Minimize stress.
If gum pain endures or if signs of an infection become apparent, seek dental consultation without delay.
Sources
- https://my.clevelandclinic.org/health/diseases/21482-gum-periodontal-disease
- https://www.nidcr.nih.gov/health-info/gum-disease
- https://www.mayoclinic.org/diseases-conditions/gingivitis/symptoms-causes/syc-20354453
- Grender, J., et al. (2020). An 8-week randomized controlled trial comparing the effect of a novel oscillating-rotating toothbrush versus a manual toothbrush on plaque and gingivitis. International Dental Journal, 70, S7–S15. https://doi.org/10.1111/idj.12571
- Sutor, S., et al. (2025). Effect of a powered and a manual toothbrush in subjects susceptible to gingival recession: A 36-month randomized controlled clinical study. International Journal of Dental Hygiene, 23(1), 26–36. https://doi.org/10.1111/idh.12834
- Xie, S., et al. (2024). Stannous fluoride protects gingival keratinocytes against infection and oxidative stress by Porphyromonas gingivalis outer membrane vesicles. Frontiers in Dental Medicine, 5, 1492369. https://doi.org/10.3389/fdmed.2024.1492369
- Zou, Y., et al. (2024). A meta-analysis comparing toothbrush technologies on gingivitis and plaque. International Dental Journal, 74(1), 146-156. https://doi.org/10.1016/j.identj.2023.06.009


