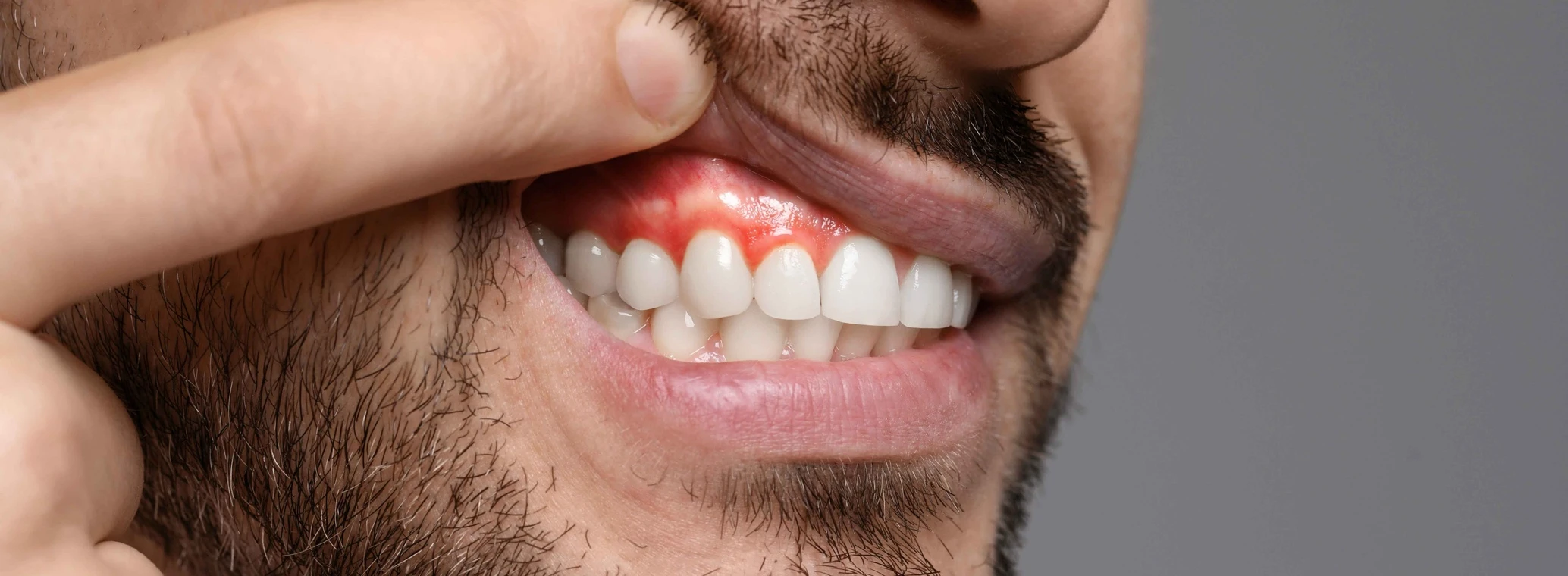
Gum Health
Gum Surgery: Types, Procedure, Recovery, and Aftercare
Hearing that you need gum surgery can feel overwhelming, but gum procedures are often the best way to rebuild your smile and safeguard your oral health. Whether you’re facing gum recession, moderate to advanced periodontal disease, or cosmetic concerns that affect your confidence, understanding the different gum surgery types, what happens during a gum surgery procedure, and how to care for your mouth afterward can make the process far less intimidating. With the right information, gum graft surgery or other treatments can help you smile comfortably and confidently again.
Key Takeaways
TABLE OF CONTENTS

TABLE OF CONTENTS
What Is Gum Surgery?
Gum surgery is an umbrella term for several procedures designed to correct gum problems. These include gum recession, where the gum tissue pulls back from the teeth. As the gums recede, more of the tooth or its root is revealed, increasing sensitivity and the risk of root decay, wear, and damage. A gum surgery procedure can treat both periodontal disease and cosmetic issues. It is most often performed by a periodontist, a dental specialist focused on preventing, diagnosing, and treating gum (periodontal) disease, as well as placing dental implants. This specialist can determine which gum surgery option is best for restoring your oral health and appearance.
Types of Gum Surgery
Gum Grafting (Soft Tissue Grafting) Gum graft surgery is frequently recommended for patients with gum recession. This gum recession surgery is designed to cover exposed roots, decrease sensitivity, and create a more even gumline.
Common gum graft surgery types include:
- Connective Tissue Graft: Tissue is collected from the roof of your mouth and placed beneath the existing gum at the recession site, then stitched into position.
- Free Gingival Graft: A thin piece of tissue is taken from the palate (roof of the mouth) and directly attached to the recessed area.
- Pedicle Graft: Gum tissue is gently repositioned from an area right next to the recession to cover the exposed root.
- Process includes:
- Carefully trimming away diseased or enlarged gum tissue
- Contouring the remaining gums for a more natural shape
- In some cases, reshaping underlying bone, usually as part of a more extensive surgery like periodontal flap surgery
- Recovery: Healing from this type of gum surgery is typically quick. Most patients can return to normal activities in just a few days.
- Procedure involves:
- Removing a small amount of gum tissue
- Sometimes reshaping the supporting bone to reveal more of the tooth’s surface
- Procedure involves:
- Gently lifting the gums away from the teeth to access and remove tartar and bacteria from deep pockets
- Smoothing the bone to remove rough areas where bacteria can collect
- Repositioning the gums tightly around the teeth to reduce pocket depth
- Benefits:
- Decreased swelling and discomfort compared to traditional gum surgery procedures
- Shorter gum surgery recovery time
- Preservation of more healthy gum tissue
What to Expect When Getting Gum Surgery
Before your gum surgery, the periodontist will review your diagnosis, explain the recommended gum surgery type, answer your questions, and provide preparation instructions.
- Most gum surgeries are carried out under local anesthesia, so the area is numb and you should not feel pain during the gum surgery procedure. Sedation can also be used if you are anxious or need a more extensive treatment.
- The length of your appointment usually ranges from one to two hours, but it may be longer depending on the complexity of your gum disease or recession.
- After the procedure, you will receive detailed post-operative instructions. These may include taking prescribed medications as directed, using antimicrobial mouth rinses to lower infection risk, and avoiding certain foods and activities to allow the surgical sites to heal properly.
Recovery and Aftercare
Successful gum surgery recovery relies heavily on proper aftercare. Healing generally happens in two phases: immediate and long-term care.
-
Immediate Post-Operative Care
- Pain Management
- Some soreness or tenderness is expected after gum surgery.
- Over-the-counter pain relievers or medications prescribed by your periodontist can help keep you comfortable.
- Swelling and Bleeding
- Mild swelling and light bleeding are normal in the first day or two.
- Applying a cold compress on the outside of your face in short intervals can help limit swelling.
- Dietary Restrictions
- Stick to soft foods and avoid anything hot, spicy, crunchy, or hard that might irritate the surgical area.
- Do not drink through straws, as the suction can disrupt clots and interfere with healing.
- Oral Hygiene
- Continue brushing your teeth gently, staying away from the surgery site unless your periodontist says otherwise.
- Use an antimicrobial mouthwash as directed to keep the area clean and reduce bacteria.
- Pain Management
-
Long-Term Care
-
Follow-Up Appointments
- Attend all scheduled visits so your periodontist can track your gum surgery recovery, remove sutures if necessary, and address any issues early.
-
Avoid Tobacco
- Smoking and other tobacco use can slow healing and increase the risk of infection or gum surgery complications.
-
Maintain Oral Hygiene
- Keep up a thorough oral hygiene routine with regular brushing and flossing.
- Avoid brushing directly over the surgical site until your periodontist confirms it is safe to do so.
-
Watch for Complications
- Contact your periodontist promptly if you experience significant or worsening pain, continuous bleeding, fever, or pus, as these can signal an infection or other problem after gum surgery.
-
Follow-Up Appointments
Summary
Gum surgery includes several different procedures used to correct gum recession, treat periodontal disease, and improve cosmetic concerns. By learning about the various gum surgery types such as gum graft surgery, gingivectomy, crown lengthening, periodontal flap surgery, and LANAP as well as what happens during a gum surgery procedure and what gum surgery aftercare involves, you can feel more informed and confident. A periodontist, a dentist who specializes in diagnosing, preventing, and treating gum disease, will help you determine which treatment is best for your condition. Each approach offers unique benefits, whether the goal is to cover exposed roots, remove diseased tissue, reshape the gumline, or manage advanced gum disease. When the right treatment is combined with careful gum surgery recovery and ongoing oral hygiene habits, your gums and teeth can become healthier, and you can enjoy a stronger, more attractive smile.
Maintaining Your Smile After Gum Surgery
Once your gum surgery is complete, adopting a gentle but effective long-term oral care routine is vital to protect your results and support your restored gum health. After your periodontist confirms that your mouth has healed enough to resume normal cleaning, using the right at-home tools can help reduce the need for additional gum recession surgery in the future. A customized daily routine can help preserve your dental work and maintain a resilient smile:
- Brush twice daily with toothpastes containing stannous fluoride. The Crest Gum Detoxify line is uniquely formulated to target and neutralize the harmful plaque bacteria that accumulate around the gumline, aiding in both treating and preventing gingivitis.
- Rinse twice daily with mouthwash, such as Crest Pro-Health Multi-Protection Mouthwash, which is clinically proven to offer 24-hour protection against plaque and gingivitis when used twice daily.
- When you brush with Oral-B iO electric toothbrushes, their gentle micro-vibrations and smart pressure sensor help you achieve an effective clean while simultaneously protecting your gums. A study demonstrated that for individuals prone to gingival recession, an electric toothbrush proved to be a safe choice over a 36-month period.
- Selecting the right brush head also significantly contributes to effective cleaning without causing gum irritation. Therefore, complement your toothbrush with an advanced brush head, such as the Oral-B iO Gentle Care, which is specifically designed for a gentle yet highly effective clean along the gumline.
- Seek a floss that resists shredding and glides effortlessly into constricted areas, such as Oral-B Glide Pro-Health Comfort Plus Floss.
TABLE OF CONTENTS

TABLE OF CONTENTS
WE RECOMMEND
Frequently Asked Questions (FAQs)

How painful is gum surgery?
During gum surgery, local anesthesia numbs the treatment area, so you should not feel pain while the procedure is being performed. Once the anesthetic wears off, it’s common to notice mild soreness, swelling, or slight bleeding, but your periodontist will provide medications and detailed post-operative instructions to reduce discomfort and help you manage recovery.

How long does gum surgery take to heal?
Initial gum surgery recovery usually takes about 1–2 weeks, though complete healing and full tissue integration can take several weeks to a few months. The exact timeline depends on the specific gum surgery type, how many areas were treated, and your personal healing response.

What are the disadvantages of gum surgery?
- Although gum surgery provides substantial benefits for your oral health, there are some potential drawbacks to consider:
- Temporary pain, bleeding, and swelling are common but usually easily controlled. Any severe or prolonged symptoms should be reported.
- As with any surgery, there is a small risk of infection, which can be minimized with proper surgical technique and careful aftercare.
- Rarely, graft tissue may not integrate properly, or healthy gum tissue can be damaged.
- Tooth sensitivity may increase temporarily as gums heal and settle into their new position.
- Changes in gum shape and position can alter the appearance of your smile.
- In very rare cases, nerve damage may affect taste or cause numbness.
- Recovery can require several days to weeks, which some patients find inconvenient.

Can receding gums be fixed without surgery?
- Mild gum recession can sometimes be managed without gum recession surgery. Non-surgical options may include:
- Scaling and root planing to deep-clean plaque and tartar from above and below the gumline, addressing the underlying cause of gum recession.
- Topical antibiotics placed on the gums or under the gumline to help control infection.
- Dental bonding to cover exposed roots and reduce sensitivity.
- The Pinhole Surgical Technique™, a minimally invasive surgical approach that repositions existing gum tissue over exposed roots without taking graft tissue from the roof of the mouth
- Smoking can impair healing and increase the risk of complications
Sources
- https://my.clevelandclinic.org/health/treatments/23504-gum-graft-surgery
- https://my.clevelandclinic.org/health/treatments/24749-gingivectomy
- https://www.mayoclinic.org/diseases-conditions/periodontitis/diagnosis-treatment/drc-20354479
- https://www.perio.org/for-patients/periodontal-treatments-and-procedures/surgical-procedures/
- https://my.clevelandclinic.org/health/treatments/16914-oral-hygiene
- https://www.dentalhealth.org/pages/category/treatments-and-procedures?take=17&Take=17
- https://www.deltadental.com/us/en/protect-my-smile/procedures.html
- https://www.nhs.uk/live-well/healthy-teeth-and-gums/dental-treatments/
- He, T., et al. (2025). Randomized Controlled Trials Assessing Exposure Frequency Effects of Stannous Fluoride on Gingivitis. JDR Clinical and Translational Research, 10(2), 124–134. https://doi.org/10.1177/23800844241263031
- Sutor, S., et al. (2025). Effect of a powered and a manual toothbrush in subjects susceptible to gingival recession: A 36-month randomized controlled clinical study. International Journal of Dental Hygiene, 23(1), 26–36. https://doi.org/10.1111/idh.12834
- Thurnay, S., et al. (2022). A Global, In-Market Evaluation of Toothbrushing Behaviour and Self-assessed Gingival Bleeding with Use of App Data from an Interactive Electric Toothbrush. Oral Health & Preventive Dentistry, 20, 1–10. https://doi.org/10.3290/j.ohpd.b2572911
- Zou, Y., et al. (2024). A meta-analysis comparing toothbrush technologies on gingivitis and plaque. International Dental Journal, 74(1), 146-156. https://doi.org/10.1016/j.identj.2023.06.009


